
Growth is important for urgent cares. To stay competitive and meet your revenue goals each year, keeping up with the evolving needs of patients is key. Sometimes that also means expanding your footprint. And according to Experity’s data on the huge increase in first year revenue, now is the perfect time to scale. Before you make any concrete plans, it’s important to set yourself up for success. We’ve learned the most common mistakes that urgent care owners make when attempting to scale through decades of consulting. Any of these can stall or prevent breaking even. Here are ten common mistakes you should avoid.
Chapter One
There are many factors to consider for site selection, especially when you’re building additional clinics. And in an increasingly crowded market, it is critical to do your homework and be savvy about where you decide to expand.
If you’re ready to scale, you probably already have a successful clinic, and presumably did great research to choose that site. There are many advantages to building scale in a given market versus spreading out. When you create more coverage in an area, you can start building economies of scale — and spend money more efficiently. Some things to consider:
If you build sites close enough to each other, you can have a bench of providers and staff that travel to the different locations based on need. This is not only easier for you, but also makes the patient experience more consistent across locations.
With clinics in a closer proximity to each other, you can pool your advertising budget for more expensive mass marketing like television and radio ads. Larger marketing efforts will also make you more recognizable and help you build your brand.
Much like staffing, if your clinics are local to one area, you can use one management team. Once you expand to another region, you need separate management teams. This is not only more costly, but also harder to maintain consistency with brand and internal culture.
When you expand within a single market, be geographically strategic in relation to your competitors. By setting up in the right locations, you can cut off your competition so your market share is not so diluted.
Consumers generally travel from less dense to more dense areas.
A couple ways you can use this to your advantage:
Think about any business hub that gets a lot of traffic. Big box stores, grocery stores, and a variety of other shopping center tenants form the core of the hub and attract customers. Your urgent care center may also be there. Now imagine the major roads that lead into these business-dense areas. If you position your urgent care centers at the entrance of these business-rich zones, you’re the first center any traveler sees on the way in from any direction — boxing in the urgent cares at the center of the hub. This makes you the most visible and accessible center from the residential communities surrounding the hub. Your competitors are left with the less-convenient, business-dense areas where no one lives.
Flanking works similarly to boxing in, but rather than setting up within an urban mecca, you create a periphery around the city. This gives you better access to people driving into a metro from the growing exurbs — those towns that are just beyond metropolitan suburbs. For episodic care, the shorter the drive, the better.
Chapter Two
Whether you expand within your state or aspire to grow nationally, you may run into challenges adding locations to your existing contracts. Sometimes you can just call the insurance company to say you’ve added a new site, but not all payers allow location additions. You could be forced to go with a different mix of insurers across clinics, which creates confusion among patients as to which of your centers is in- or out-of-network with their insurance.
When you want to expand into new geographies, it’s important to know up front whether you understand the reimbursement and contracting rules within those states. Always research open/closed networks, physician onsite requirements, current rates, etc., before investing in a new location.
Chapter Three
Urgent care is considered on-demand healthcare. Patients see their urgent care options in the same way they look at other on-demand services like shopping and dining. Yet the public can’t tell most urgent care centers apart.
If you want to beat out your competitors and establish long-term success, you need to think about your brand in terms of retail differentiation. In other words, you don’t want to just be one more “doctor’s office;” you want to provide a unique healthcare experience — in a way that is specific to you and what you’re best at.
To create a brand, start by answering some questions:
The Journal of Urgent Care Medicine (JUCM) published Alan Ayers’ article, “A Process Approach to Differentiating Your Urgent Care Brand by Ensuring that Patients Leave Satisfied,” in which Ayers explains:
“Developing a differentiated brand takes planning, which entails designing processes, systems, and training that result in an exceptional patient experience. For most urgent care centers, pertinent touchpoints can be loosely grouped into [six] categories.” Consider these categories through a patient’s eyes:
Ayers sums up urgent care branding nicely:
“In short, a brand is a promise. Established brands declare their promise explicitly, and they reinforce that promise at every possible touchpoint. Whether it is a promise of the highest quality, lowest prices, greatest convenience, or most novel experience, a touchpoint is the vehicle that brands employ to capture market share. For urgent care operators seeking to build the kind of regional or national brand loyalty that helps them stand out from the pack, there must be a definitive and forward-thinking process approach undertaken to shape their brand’s touchpoints.”
Chapter Four
While your brand is the outward reflection of who you are as a company, your culture is the inward expression. Culture not only supports your brand, but also improves morale to improve employee job satisfaction and attract and retain top-tier new hires.
To ensure you have a remarkable culture that lasts — especially one that is focused on the patient — you must assess whether the staff understands your brand and is clear on expectations, feels safe to speak up, and is recognized for a job well done.
Ultimately, you want to set expectations that engage employees in the right things. People often say they go into health care because they “want to help people.” If they are engaged in goals around the patient experience, they will live the culture you establish.
Remember, culture must be consciously built by providing the environment that fosters the values you want your staff to exhibit day in and day out. If your current culture is not clearly defined based on set goals and expectations, you won’t have consistency across your clinics.
Your expectations should not only be how to treat patients, but also how to treat coworkers, and what it means to be a good team player and employee. Additionally, you need to measure performance and provide feedback. When they’re doing a good job, tell them. When team members struggle, help them win. And if an employee cannot meet expectations — when possible — consider a better-suited role before resorting to termination.
All of this supports a culture of celebrating wins. Not only do employees need to hear praise from leaders, but they should also be encouraged to celebrate each other. Give staff the ability to recognize each other. There are various reward program models available that allow employees to recognize one another and win prizes or redeem points. Learn more about reward programs shared in our team culture webinar >>
Another important component of a positive culture is giving grace. Humans will make mistakes. You and your staff should demonstrate grace when challenges arise. Of course, that doesn’t mean you should keep an employee in a role that is not a fit. But if employees know they can admit fault without enduring a harsh backlash, they’ll be more likely to own mistakes — which results in faster resolution and a better learning and working environment.
High-level tips to set expectations that influence a great culture:
Chapter Five
The number one reason urgent cares fail (close permanently) is running out of money — your working capital. All the cash needed to make payroll, buy supplies, pay rent, and fund business operations comes out of your working capital. And for a mature clinic, sales revenue provides that working capital. But for a new clinic that has not yet reached a breakeven point, this capital comes from bank loans and owner equity.
So the problem arises when owners underestimate the amount of cash they need or time it will take to break even. And this is a fluid timeline in urgent care. While it used to take an average of nearly a year to become profitable, post-COVID averages are drastically shorter. Keep current with this data to set realistic goals. You can find current statistics in the most recent copy of Experity’s Urgent Care Quarterly (UCQ).
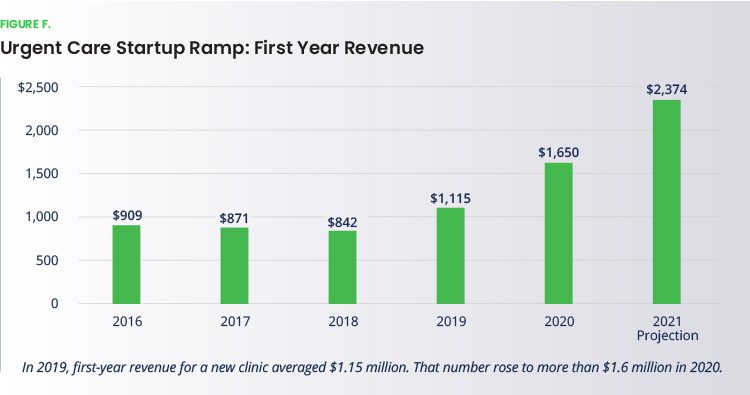
Even in a market that becomes profitable quickly, it’s important to consider the factors that can cause a delay in achieving breakeven profitability:
To avoid exhausting working capital, it’s imperative when creating a network of clinics to accurately project how much money the operation will require — not only the costs of building out and opening the center, but also the costs of staying in business until there is sufficient patient revenue to cover the center’s overhead. The baseline operating metrics of your existing urgent care should help you make accurate projections so you can conservatively manage cash by controlling expenses, having a reserve or credit line available, and developing sound business plans.
If you need help creating a new or revising your existing business plan, we recommend Ayers’ JUCM article, “If Your Business Doesn’t Work on Paper, it Won’t Work in Reality.”
Chapter Six
As you scale your business, it’s important to approach it as one operation across all locations. In other words, don’t leave processes up to each individual clinic. Aside from it being a nightmare to manage, you cannot deliver a consistent brand experience if clinics operate autonomously.
Furthermore, if you have any floating staff members, it will be far more efficient for them to go from one clinic to another if your layouts are similar — so they don’t have to rummage through cupboards or hunt down equipment to complete tasks.
Staff will also appreciate knowing that the expectations, KPIs, workflows, and other protocols are the same in every clinic. But most importantly, patients can visit any location and receive the same quality of care.
In short, you should create an operational playbook that is:
And it should also take into account:
Your center’s operating philosophy and culture should be centered around highly optimized processes. Aim to improve workflows that boost patient throughput; eliminate unnecessary administrative burdens for providers and staff; and identify/correct errors, friction points, and bottlenecks at every opportunity. Here are some guiding principles to build your workflows and processes:
When it comes to a patient’s perception of urgent care services, the bar is not set against other healthcare environments. Patients compare their experience at your urgent care with that of restaurants, retail, and any other service they pay for. They expect convenience, affordability, and great service with minimal wait and hassle. Which means that urgent care facilities need to be champions of patient engagement at every level: digital, face-to-face, and the visit itself. Some no wait, no waste, no hassle optimizations for the patient experience include:
Having an engaged, empowered employee culture is critical to the success of the other two pillars. All cultures — successful or unsuccessful — begin and end with the quality of its people, and their commitment to the success of the organization. Here are some ideas on how to keep your staff motivated, engaged, and empowered:
If you want to explore these ideas further, Creating the ‘Ideal’ Urgent Care Experience provides in an-depth explanation of the pillars and principles outlined above.
Chapter Seven
With one or two locations, you may have an excellent billing person, nurse, or other staff members who have the experience to excel at their jobs. But once you hit three locations, you’re now dealing with a complexity of issues that may be beyond the skillset and expertise of your original team.
What often happens in these situations is that well-meaning loyalty prevents the owner from hiring HR, operations, and finance professionals who are better qualified to tackle the more sophisticated, large-scale issues.
This not only disables you operationally, but it also burdens the staff who are trying to keep up. They used to feel successful in their jobs, but now they feel incompetent and stressed — which can create a cycle that hurts both them and your clinic.
Chapter Eight
Much like how a pilot flying through bad weather depends on his or her instrument panel to know their positioning, direction, and speed, you need to be able to measure how your business is performing against your goals, industry trends, and everything else that impacts your success.
Key performance indicators (KPIs) are quantifiable business metrics that gauge various aspects of business performance over time. They provide insight to an organization’s financial health, and spotlight organizational strengths and weaknesses. You should also use KPIs to set strategic and organizational goals, and to routinely measure your company’s performance against industry benchmarks.
While every clinic will determine its own metrics, here are ten of the most important KPIs to watch in your urgent care.
KPI #1
The average revenue per visit is the total amount received per visit from both the patient and the payer. Average revenue shows actual payments received per visit. It also helps determine projected cash amounts.
KPI #2
E/M code distribution shows the use of code levels by staff. E/M codes directly affect reimbursement amounts. Code levels 1 through 5 tell payers the level of visit complexity, and dictate the charges for services rendered.
KPI #3
Ancillary revenue per visit is how much revenue you receive per visit for procedures and services above the cost of the visit. Urgent cares often have a contracted amount for an office visit E/M code with payers — so ancillaries are in addition to that amount. Ancillary charges can be labs, injections, x-rays, or medical equipment.
KPI #4
Front desk collection rate is the percentage of collections gathered by the front desk from patients before they leave the clinic. A larger percentage captured at the front desk is typically reflected in a higher percentage of overall collections per visit.
KPI #5
Days in A/R is the amount of time your charges are sitting in accounts receivable. This is the revenue you have yet to get paid for, divided by the average daily charges at your clinic. The lower your days in A/R, the quicker the turnaround for reimbursement.
KPI #6
This metric is the percentage of A/R being held for over 120 days. The longer your A/R isn’t collected (in 90 to 120+ days) the more likely it is you have serious collection issues — and lower overall reimbursement rates.
KPI #7
Days to bill is how long it takes your billing team to get claims submitted. Faster days to bill means fewer days in A/R and faster reimbursement from insurance and patients. However, faster days to bill is not worth causing claim quality to suffer. If speed is causing an increase in claim rejections, it means more days in A/R and slows the revenue cycle.
KPI #8
Days to pay is the amount of time it takes a payer to pay a claim. Quicker reimbursement means fewer days in A/R and faster revenue realized.
KPI #9
The best payer contract rates won’t matter if you don’t have any patients coming through the door. You won’t reach a profit without adequate patient volume. An urgent care business plan should designate breakeven and profit points tied to visits per day.
KPI #10
This is the amount of time it takes from the moment a patient enters your clinic to when they leave. In urgent care, lower door-to-door times increase the number of patients you can see. The more efficient the visit time, the more revenue opportunities.
To understand what affects these KPIs and how to measure them, download 10 KPIs to Watch in Your Urgent Care.
Chapter Nine
Urgent care is no longer an “if you build it, they will come” industry. According to Andrew Ibbotson, Vice President of the National Research Corp. in Nebraska, “Urgent care traffic is driven more by online search results, geography, wait times, and availability than traditional healthcare delivery.” These nuances make identifying the most effective marketing strategies for your urgent care clinic even more vital to success.
While digital marketing and advertising is essential today, there is still value in more conventional tactics. When you grow your footprint, your marketing budget will become big enough to leverage marketing outlets that will increase your exposure — if you expand the right way. The key here is to invest strategically, which gets easier the closer together your clinics are located. Again, it’s very difficult for a single clinic to buy much exposure, but a localized footprint of centers can purchase billboard space, mass media ads, and even better extend grass-roots campaigns. While these cost more, you get more mileage from, say, one billboard that advertises three or four locations.
Ideas and concepts for urgent care marketing is another topic too big to detail here. Learn how to get the most out of your marketing by reading Urgent Care Marketing 101.
Chapter Ten
Cap ex, or capital expenditure, includes the cost of the building, renovations, furniture, fixtures, and equipment. Traditionally, the mistake has been to spend too much — the more of your capital you sink into this area, the longer it takes to break even. Additionally, it limits the number of locations you can add.
More recently, we’ve seen people spend too little on cap ex by opening pop-up clinics. They’re taking the extra revenue that COVID-19 generated and investing in these smaller clinics — most of which don’t have the full capabilities of a traditional urgent care, like radiology. The risk here is that once COVID-19 tests and vaccinations wane, these centers won’t be able to offer enough of the services that normally keep them afloat.
Scaling your footprint is exciting and can be very profitable when done correctly. However, many clinics struggle because it is such a huge undertaking. If you want to scale confidently, lean on experts to help you through the entire process.
Experity’s consulting team has decades of experience and industry expertise that has helped hundreds of urgent care clinics meet their true growth potential. Because we’re a part of the only HIT company that offers connected solutions solely for urgent care, we have the data and the expertise to help you make the best decisions for your business. Learn more about our services here or schedule a consultation.